Peri-implantitis is a serious inflammatory condition around dental implants that can lead to bone loss and, if not managed properly, implant failure. Clinically, it is different from gum disease around natural teeth because it affects the bone supporting an artificial implant, which does not have the same biological attachment system as natural teeth (clinical consensus, implant dentistry).
As noted in implant dentistry practice (Dr Ahmed, clinical guidance), home care alone cannot fully treat peri-implantitis once bone loss has started. Professional treatment is the only definitive way to stop disease progression, while home care plays a supportive role only.
What is peri-implantitis (clinical definition)
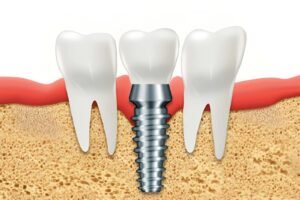
Peri-implantitis is a biofilm-induced inflammatory disease affecting the soft tissue and supporting bone around a dental implant. It typically develops after an earlier stage called peri-implant mucositis, which is reversible inflammation of the gums around the implant (clinical consensus, Dr Ahmed).
If untreated, peri-implant mucositis can progress to peri-implantitis, where:
- Bone around the implant is destroyed
- Gum tissue recedes
- The implant may loosen over time
This is not the same as standard gum disease (periodontitis) because the implant lacks a periodontal ligament, making bone loss often faster and more difficult to control once established (implant dentistry clinical guidance).
Signs and symptoms of peri-implantitis
Early detection is critical. Common signs include:
- Red or swollen gums around the implant
- Bleeding when brushing or probing
- Persistent bad taste or bad breath
- Gum recession around the implant
- Pain or discomfort when chewing
- In advanced cases, implant mobility (looseness)
Causes and risk factors
Peri-implantitis is primarily caused by bacterial plaque accumulation (biofilm infection) (clinical consensus).
Key risk factors include:
- Poor oral hygiene (main cause)
- Smoking (significantly increases risk and reduces healing capacity)
- History of gum disease
- Poor implant positioning or cement remnants
- Uncontrolled diabetes or systemic inflammation
Can peri-implantitis be treated at home?
No — once peri-implantitis is established, home care cannot cure it.
Home care can only:
- Slow progression
- Reduce bacterial load
- Support professional treatment outcomes
Definitive treatment requires professional decontamination, possible antibiotics, and sometimes surgical intervention depending on severity.
Professional treatment (the only definitive fix)
As clinically noted by implant specialists, treatment may include:
- Deep cleaning around the implant (subgingival debridement)
- Mechanical removal of biofilm
- Antiseptic irrigation
- Local or systemic antibiotics (in selected cases)
- Surgical flap treatment for advanced bone loss
- In severe cases, implant removal
👉 Home care alone is not sufficient once bone loss is present.
Home care that SUPPORTS treatment (not a cure)
These measures help control bacteria and support professional care:
1. Brushing technique
Use a soft-bristled toothbrush twice daily, gently cleaning around the implant.
2. Interdental cleaning
Use soft interdental brushes or implant-specific floss daily to remove plaque between teeth and implants (periodontal hygiene guidance).
3. Chlorhexidine mouthwash (0.12%)
Short-term use of chlorhexidine 0.12% mouthwash may reduce bacterial load around implants (clinical standard guidance).
⚠️ Long-term use is not recommended unless prescribed due to staining and taste alteration.
4. Oral irrigation
Low-pressure water irrigators can help flush food debris and plaque from hard-to-reach areas (supportive hygiene method).
5. Lifestyle control
- Stop smoking (the strongest modifiable risk factor)
- Maintain controlled blood sugar if diabetic
- Follow a balanced diet supporting gum healing (clinical consensus)
Warning signs of emergency peri-implantitis
Seek urgent dental care immediately if any of the following occur:
- Pus discharge around the implant
- The implant feels loose or moves
- Severe, worsening pain
- Facial swelling or spreading infection
- Fever or feeling unwell
These signs may indicate active infection and advanced bone loss, requiring urgent intervention.
Prevention
Preventing peri-implantitis is far more effective than treating it (clinical consensus):
- Maintain strict oral hygiene daily
- Use interdental brushes around implants
- Attend regular dental check-ups and professional cleaning
- Avoid smoking entirely
- Address early gum inflammation immediately
Conclusion
Peri-implantitis is serious. But with good oral hygiene and the right home remedies, you can manage it well. Remember to brush and floss every day. Use antimicrobial mouthwash. Also, keep a healthy lifestyle. Regular dental check-ups are crucial to keep your implants in good shape. If you notice any signs of infection, seek professional help promptly. Follow these steps. They will ensure the long-term success of your dental implants and a healthy smile.
Contact Old Town Dental Care
If you need professional advice or treatment for peri-implantitis, Old Town Dental Care is here to help. Our experienced team is dedicated to providing top-quality dental care to ensure your implants remain healthy and secure. Don’t wait—contact us today to schedule a consultation and take the first step towards optimal oral health.
Frequently Asked Questions
Can peri-implantitis be reversed at home?
Yes, early peri-implantitis (peri-implant mucositis) can often be fixed at home with good oral hygiene. This includes brushing, flossing, and using antimicrobial mouthwash.
How often should I rinse with saltwater for peri-implantitis?
Rinse with saltwater twice a day. This can help soothe inflamed gums and reduce bacteria around the implant.
Is smoking a major risk factor for peri-implantitis?
Yes, smoking significantly increases the risk of peri-implantitis and can slow the healing process. Avoid tobacco products to maintain good oral health.
What type of mouthwash is best for peri-implantitis?
Use an antimicrobial mouthwash containing chlorhexidine. It is effective in reducing bacteria and preventing infections around dental implants.
When should I seek professional help for peri-implantitis?
Seek professional help if symptoms persist or worsen. Also, seek help if you see pus around the implant, if the implant becomes loose, or if you have severe pain or swelling.
Last Updated: April 2026